Colorectal adenomas and MAFLD: a cross-sectional study in a Hispanic screening cohort
Abstract
Aims: Prior evidence demonstrates an association between non-alcoholic fatty liver disease (NAFLD) and colorectal adenomas (CRA) risk. However, information using the new definition of the disease [i.e., metabolic dysfunction-associated fatty liver disease (MAFLD)] is scarce. We aimed to assess the relationship between MAFLD and CRA risk.
Methods: We conducted a cross-sectional study including patients from three university centers in Chile who underwent a colonoscopy for colorectal cancer screening and abdominal imaging study. We obtained sociodemographic and clinical data, and we performed univariate and multivariable regression analyses.
Results: In total, 895 patients were included; 42% were male, the mean age was 59.9 ± 9.3 years, and 37.8% (338) had CRA. Patients harboring polyps were predominantly males (48.2% vs. 38.2%, P = 0.002), older (61.6 ± 8.7 years vs. 58.9 ± 9.5 years, P < 0.001), and exhibited a higher body weight than controls [75 (66-88) kg vs. 72 (63-82.3) kg, P = 0.002]. Fifty-six percent of patients showed hepatic steatosis in imaging studies and 54.4% met MAFLD diagnostic criteria. The adenoma detection rate was higher in the MAFLD group compared to controls (46.4% vs. 27.5%, P < 0.001). In the multivariable analysis, MAFLD was significantly associated with the presence of CRA (odds ratio = 2.32; 95%CI: 1.68-3.19, P < 0.0001). There were no statistically significant differences of histopathological characteristics of the adenomas according to the presence of MAFLD.
Conclusion: The present study shows that, in Chilean Hispanic subjects, MAFLD is associated with an increased risk of CRA. This information may be useful to design specific screening colonoscopy recommendations in MAFLD patients.
Keywords
INTRODUCTION
Colorectal cancer (CRC) is considered a public health priority since it is the third most common cancer with the second highest mortality worldwide. CRC was responsible for more than 9.6 million deaths in 2018[1]. Data from Latin America are also worrisome, as the burden of CRC in the region has increased in recent years[2]. In Chile, CRC is the second most frequent cancer and has exhibited a rise in incidence and mortality curves in recent years[3].
Most CRC cases (70%) follow the adenoma-carcinoma sequence where premalignant lesions are represented by colorectal adenomas (CRA)[4]. The rest of the cases develop through the “serrated pathway” or from dysplasia secondary to chronic inflammation in patients with inflammatory bowel disease[5]. Polyps are the clinical manifestation of altered cell proliferation processes that originate in the colorectal epithelium and are recognizable by endoscopic studies[6]. They are classified into those with no malignant neoplastic potential, such as inflammatory and hyperplastic polyps, and those that may originate a CRC, such as CRA. In addition, CRA can be classified into low- and high-risk lesions according to size, degree of dysplasia, and the presence of a villous component[7].
CRC can be prevented by controlling risk factors or through endoscopic resection of polyps[8]. Different screening methods to detect adenomas have been shown to reduce CRC incidence as well as CRC-associated mortality. These include non-invasive tools, based on testing for occult blood in the stools, and invasive procedures such as colonoscopy[9,10]. Current screening recommendations made by scientific societies are constantly being updated in light of new evidence. Of note, the recent rise of CRC in the younger population led to reducing the age to start screening from 50 to 45 years[11]. Other updates seek to ensure minimum standards of care that have shown benefit in reducing cancer rates in the intervals between colonoscopies, such as an adenoma detection rate (ADR) > 25%[12].
Nonalcoholic fatty liver disease (NAFLD) affects more than one-quarter of the adult population worldwide and is closely linked to underlying metabolic syndrome, obesity, and type 2 diabetes[13]. Several studies have shown that NAFLD is associated with increased incidence of multiple neoplasms, including hepatocarcinoma and breast cancer, among others[14]. In addition, NAFLD is also associated with an increased risk of CRA and CRC[15,16]. Thus, NAFLD constitutes an emerging risk factor for CRC.
A process of NAFLD renaming is ongoing and the term metabolic dysfunction-associated fatty liver disease (MAFLD) has been recently proposed[17]. This name change emphasizes metabolic dysfunction in NAFLD and suggests the implementation of positive diagnostic criteria[17,18]. Although NAFLD and MAFLD are not completely overlapping, most of the available knowledge on NAFLD could be extrapolated to MAFLD, but more research is needed in this regard. Despite the notable impact of NAFLD in CRC, there are no data from Hispanic populations assessing the influence of MAFLD on the risk of CRA. In the present study, we explored the existence of an association between the presence MAFLD and the existence of CRA in patients attending to screening colonoscopy at three university centers in Chile.
METHODS
Ethical approval
This study was approved by the Institutional Review Board (Pontificia Universidad Católica de Chile, Santiago, Chile; ID: 210309004).
Data collection
We conducted a cross-sectional study including individuals from three university centers, which are part of the Healthcare Network of the Pontificia Universidad Católica de Chile School of Medicine: Red de Salud UC-CHRISTUS Hospital (Santiago, Chile), the Clínica UC San Carlos de Apoquindo (Santiago, Chile), and San Joaquín Medical Center (Santiago, Chile). All demographic information, clinical variables, laboratory results, imaging, and endoscopic and histological data were obtained from the institutional medical records by two independent observers (Villalón J and Villalón F), and disagreements were resolved by a third reviewer (Villalón A). We collected data between January 2018 and December 2020. We included patients older than 18 years, with no digestive symptoms, who underwent screening colonoscopy and an abdominal imaging study (i.e., abdominal ultrasound, abdominal computed tomography scan, or magnetic resonance imaging) in the 12 months before or after the index colonoscopy. We excluded all those with digestive symptoms (i.e., digestive bleeding, weight loss, recent change in intestinal transit time, etc.), with a prior diagnosis of cirrhosis or another chronic liver disease, with a personal history of CRC, resection of the large intestine, familial polyposis syndrome, or inflammatory bowel disease[19]. Colonoscopies without cecal intubation or suboptimal bowel preparation [i.e., Boston Bowel Preparation Scale (BBPS) score lower than 7], as defined by the operator, were also excluded[20].
We also recorded the following variables from the institutional electronic medical records: age at the time of colonoscopy, gender, weight (kg), waist circumference (cm), comorbidities (hypertension, diabetes, prediabetes, insulin resistance, dyslipidemia, sedentary lifestyle, obstructive sleep apnea-hypopnea syndrome, coronary heart disease, stroke, celiac disease, and family history of colorectal cancer), tobacco and alcohol consumption in the six months prior to colonoscopy, and medical therapy (including vitamin E, metformin, aspirin, and statins)[21-25]. The recorded comorbidities were selected to adequately diagnose MAFLD (hypertension, diabetes, prediabetes, insulin resistance, and dyslipidemia), and other conditions were chosen due to the potential association with a higher risk of CRA and CRC[26-29]. We considered the laboratory tests performed six months before or after the image. In addition, we calculated the FIB-4 score to estimate the presence or absence of liver fibrosis.
Colonoscopies with cecal intubation, BBPS score ≥ 7 points, and a withdrawal time greater than 6 min were considered as adequate quality studies. Colonoscopies were performed by either gastroenterologist endoscopists or surgeons. Initially, the presence or absence of polyps was described. Lesions were described by their morphology as pedunculated, sessile, or flat according to the Paris classification. We recorded polyp neoplastic appearance and size (according to the endoscopist’s criteria). The number of lesions found was classified as single or multiple (≥ 1). The location of the lesions was described in relation to the splenic flexure, where the colon is considered proximal from the cecum to the ascending colon, up to the transverse colon including the flexure, and the rest as distal. All polyps were analyzed by pathologists and classified according to the histological criteria of the World Health Organization. In cases where more than one polyp was found, the largest or the highest histological grade was described, the latter being the main criterion in dissenting cases. Colonoscopy findings allowed categorizing the study population into two groups (i.e., high-risk and low-risk groups). The high-risk group was defined by the presence of one or more adenomas ≥ 10 mm or the presence of an advanced adenoma (villous histology, high-grade dysplasia, or intramucosal cancer). Patients having CRA that did not meet these criteria were classified as having low risk of CRC. A colonoscopy without findings or with non-adenomatous polyps (i.e., inflammatory, hamartomatous, or hyperplastic polyps) was considered normal. In addition, we did not consider serrated polyps in the analyses.
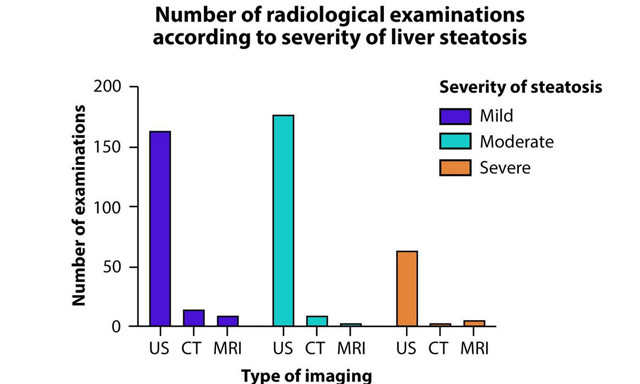
The presence and degree of hepatic steatosis were evaluated by expert radiologists. Steatosis was defined, according to the radiological technique used, based on the classic criteria such as increased echogenicity and the visualization of intrahepatic vessels and the diaphragm on ultrasound, the lower attenuation of the liver parenchyma measured in Hounsfield units on CT scan, and the loss of hepatic signal in the opposed phase images in magnetic resonance imaging[30]. Finally, the diagnosis of MAFLD was made according to recently published criteria, which are based on evidence of steatosis by imaging or histology and the presence of diabetes, obesity, or at least two minor criteria of metabolic dysfunction[29].
Statistical analysis
We evaluated the distribution of continuous variables using the Kolmogorov-Smirnov test, age being the only variable with normal distribution expressed as the mean ± standard deviation. The rest of the variables were expressed as median and interquartile ranges. The differences between the two groups were analyzed with a t-student test for age and with a non-parametric test for the rest. The categorical variables were evaluated with the Chi-square test. A statistically significant difference was considered with a P-value < 0.05. The potential variables were analyzed using logistic regression. All significant laboratory tests were reassessed on a logarithmic scale to facilitate interpreting the results. A multivariable regression analysis was conducted to assess the association between MAFLD and CRA, adjusting for potential confounders[31]. We selected variables for multivariable analysis according to significance in the univariate analysis. We constructed three models, including all the significant variables (Model 1), clinical variables exclusively (Model 2), and including only those variables that resulted significantly in Model 1 or 2 to better predict presence of CRA (Model 3 or fully predictive model). We measured the goodness-of-fit for each model using the Hosmer-Lemeshow test. Finally, we used variance inflation factors to detect collinearity between variables. We used the statistical software SPSS (IBM Corp.) v24.0 to perform all the analyses.
RESULTS
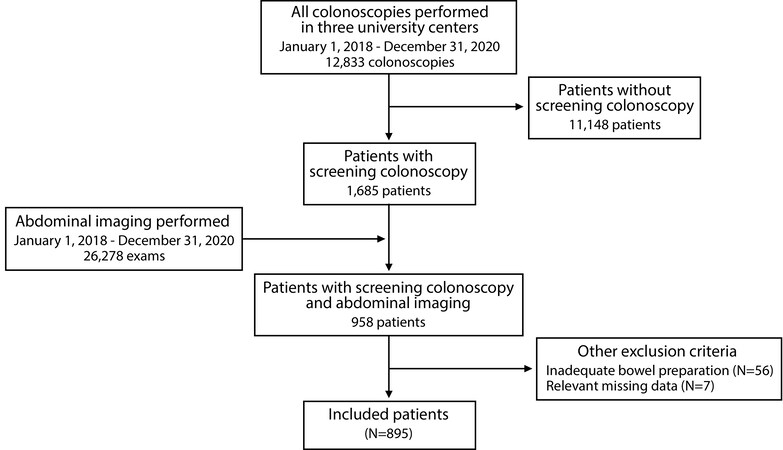
In total, 12,833 colonoscopies were performed during the period analyzed in this study. Of those procedures, 1685 were screening studies with 958 having an abdominal imaging study in the 12 months before or after the index colonoscopy. Sixty-three patients were discarded because they did not meet inclusion criteria. The flow-chart of the study population enrolled in the final analysis is summarized in Figure 1.
In total, 895 patients were analyzed. The mean age was 59.9 ± 9.3 years and 58% were female. The median weight was 73 (65-84.5) kg, median waist circumference was 98 (93-110) cm, and 82% were overweight. Fifty-six percent (501) of patients had hepatic steatosis and 54.4% (487) met the MAFLD criteria. Ultrasound was the most widely available imaging method (74.4%) to establish the presence of steatosis
Baseline characteristics of patients with and without colon adenomas
| Variable | Total population (n = 895) | Absence of adenomas (n = 557) | Adenoma detection (n = 338) | P-value |
| General characteristic Age (years) Male gender (%) Weight (Kg) | 59.9 ± 9.3 376 (42.0) 73 [65-84.5] | 58.9 ± 9.5 213 (38.2) 72 [63-82.3] | 61.6 ± 8.7 163 (48.2) 75 [68-88] | < 0.0001 0.002 0.002 |
| Comorbidities (n, %) Diabetes Prediabetes Overweight Hypertension Insulin resistance Dyslipidemia Sedentarism OSAHS Coronary artery disease Ischemic stroke Celiac disease Family history CRC Alcohol consumption Smoking | 90 (10.3) 120 (13.7) 568 (82.0) 362 (41.3) 143 (16.3) 378 (43.2) 338 (71.3) 45 (5.2) 21 (2.4) 11 (1.3) 10 (1.2) 123 (14.7) 366 (45.9) 213 (25.9) | 43 (7.9) 69 (12.6) 332 (77.8) 214 (39.1) 87 (15.9) 224 (41) 198 (70.5) 31 (5.7) 9 (1.7) 3 (0.6) 5 (0.9) 69 (13.1) 237 (47.6) 121 (23.3) | 47 (14.2) 51 (15.4) 236 (88.7) 148 (44.8) 56 (17) 154 (46.7) 140 (72.5) 14 (4.3) 12 (3.6) 8 (2.4) 5 (1.5) 54 (17.4) 129 (43.1) 92 (30.3) | 0.004 0.243 < 0.0001 0.095 0.789 0.102 0.623 0.346 0.064 0.016 0.421 0.086 0.223 0.028 |
| Current therapies (n, %) Vitamin E Metformin Aspirin Statins | 18 (2.1) 192 (22.1) 79 (9.1) 246 (28.2) | 10 (1.8) 110 (20.3) 44 (8.1) 141 (26) | 8 (2.4) 82 (25.1) 35 (10.7) 105 (32) | 0.539 0.100 0.201 0.055 |
| Radiologic liver steatosis (n,%) | 501 (56.0) | 272 (48.8) | 229 (67.8) | < 0.0001 |
| MAFLD diagnosis (n, %) | 487 (54.4) | 261 (46.9) | 226 (66.9) | < 0.001 |
| Metabolic laboratory Total Cholesterol (mg/dL) HDL-c (mg/dL) LDL-c (mg/dL) Triglycerides (mg/dL) Fasting blood glucose (mg/dL) 2-HPL glucose levels (mg/dL) Glycosylated hemoglobin (%) HOMA | 191 [163-216] 52 [42-61] 110 [87-133] 119 [88-166] 95 [88-104] 125 [97-167] 5.7 [5.4-6.0] 3.1 [2.0-4.2] | 192 [165-215] 52 [43-62] 112 [88-133] 113 [83-162] 94 [87-101] 120.5 [96-145] 5.6 [5.4-5.9] 2.9 [2.0-4.2] | 188 [159-217] 50 [42-59] 109 [85-133] 127 [95-176] 98 [90-108] 137 [109-170] 5.8 [5.5-6.1] 3.4 [2.4-4.2] | 0.586 0.331 0.296 0.002 < 0.0001 0.314 0.017 0.151 |
| General laboratory Hemoglobin (g/dL) Platelets (× 106/μL) Creatinine (mg/dL) AST (U/L) ALT (U/L) γ-GT (U/L) ALP (U/L) Total bilirubin (mg/dL) INR Albumin (g/dL) | 14.2 [13.3-15.1] 240 [201-277] 0.8 [0.7-1.0] 22 [18-26] 23 [18-35] 24 [17-38] 81 [68-98] 0.5 [0.4-0.7] 1.0 [1.0-1.0] 4.6 [4.4-4.8] | 14.0 [13.2-15.1] 240 [200-280] 0.8 [0.7-0.9] 22 [18-26] 23 [17-34] 22 [16-36.5] 80 [68-96] 0.5 [0.4-0.7] 1.0 [1.0-1.0] 4.6 [4.4-4.8] | 14.4 [13.4-15.3] 240 [200-270] 0.8 [0.7-1.0] 22 [18-27] 24 [18-35] 27 [18-40] 83 [68-100] 0.52 [0.39-0.72] 1.0 [1.0-1.0] 4.6 [4.4-4.8] | 0.020 0.819 0.010 0.842 0.246 0.024 0.470 0.054 0.181 0.310 |
| FIB-4 | 1.1 [0.9-1.5] | 1.1 [0.9-1.5] | 1.2 [0.9-1.5] | 0.878 |
| Withdrawal time (min) | 12 [10-15] | 11 [10-15] | 14 [11-16] | < 0.001 |
CRA were identified in 338 (37.8%) out of 895 patients. These patients were predominantly males (48.7% vs. 38.2% of patients without CRA, P = 0.002), older than patients without CRA (mean age 61.6 ± 8.7 years vs. 59.9 ± 9.3 years in those without CRA, P < 0.001), and had a higher body weight [75 (66-88) kg vs. 72 (63-82.3) kg in patients without CRA, P = 0.002]. Furthermore, patients with CRA had a more frequent history of diabetes (14.2% vs. 7.9%, P = 0.004), ischemic stroke (2.4% vs. 0.6%, P = 0.016), and smoking (30.3% vs. 23.3%, P = 0.028) [Table 1]. The presence of MAFLD was significantly higher in patients with CRA (66.9% vs. 46.9%, P < 0.001). Serum triglycerides [127 (95-176) mg/dL vs. 113 (83-162) mg/dL, P = 0.002], fasting blood glucose [98 (90-108) mg/dL vs. 94 (87-101) mg/dL, P < 0.001], and glycosylated hemoglobin [5.8% (5.5%-6.1%) vs. 5.6% (5.4%-5.9%), P = 0.017] were also higher in the group with CRA. The colonoscopy withdrawal time was also significantly higher in patients with CRA [Table 1]. No differences were found with respect to FIB-4 or pharmacological therapies with incidence in fatty liver and CRC chemoprophylaxis [Table 1].
The general adenoma detection rate was 37.8%, and it was higher in the MAFLD group (46.4% vs. 27.5%, P < 0.001). We compared the histopathological differences of polyps according to the presence of MAFLD, and we did not identify differences regarding location, number, morphology, size, and malignancy of the colorectal polyps between the two groups [Table 2]. In addition, we did not identify differences in the characteristics according to the presence of MAFLD when we compared adenomas exclusively [Table 3]. No statistically significant association was found between the degree of hepatic steatosis and the presence of colorectal adenomas (P = 0.458) [Supplementary Table 1].
Comparison of location, number, morphology, size, and histology of the polyps between the MAFLD vs. non-MAFLD groups
| Parameter | Total n = 439 | MAFLD group n = 284 (64.7%) | Non-MAFLD group n = 155 (35.3%) | P-value |
| Location Proximal colon Distal colon Right + left + rectum | 209 (47.6%) 128 (29.2%) 102 (23.2%) | 142 (50%) 79 (27.8%) 63 (22.2%) | 67 (43.2%) 49 (31.6%) 39 (25.2%) | 0.398 |
| Number Single Multiple | 200 (45.6%) 239 (54.4%) | 131 (46.1%) 153 (53.9%) | 69 (44.5%) 86 (55.5%) | 0.746 |
| Morphology Pediculated Sessile Flat | 36 (16.5%) 166 (76.1%) 16 (7.4%) | 20 (14.2%) 113 (80.1%) 8 (5.7%) | 16 (20.8%) 53 (68.8%) 8 (10.4%) | 0.301 |
| Size < 10 mm ≥ 10 mm | 280 (80.5%) 68 (19.5%) | 187 (80.6%) 45 (19.4%) | 93 (80.2%) 23 (19.8%) | 0.238 |
| Pathological features Non-adenoma Adenoma Non-advanced adenomas Advanced adenomas In-situ neoplasia Colorectal Cancer | 96 (21.9%) 338 (77%) 270 (79.9%) 68 (20.1%) 5 (1.1%) 0 (0%) | 54 (19%) 226 (79.6%) 182 (80.5%) 44 (19.5%) 4 (1.4%) 0 (0%) | 42 (27.1%) 112 (72.3%) 88 (78.6%) 24 (21.4%) 1 (0.6%) 0 (0%) | 0.743 < 0.001 0.672 0.217 0.471 - |
Comparison of location, number, morphology, and size of adenomas between the MAFLD vs. non-MAFLD groups
| Parameter | Total n = 338 | MAFLD group n = 226 | Non MAFLD group n = 112 | P-value |
| Location Proximal colon Distal colon Right + left + rectum | 173 (51.2%) 79 (23.4%) 86 (25.4%) | 119 (52.6%) 51 (22.6%) 56 (24.8%) | 54 (48.2%) 28 (25.0%) 30 (26.8%) | 0.742 |
| Number Single Multiple | 142 (42%) 196 (58%) | 97 (42.9%) 129 (57.1%) | 45 (40.2%) 67 (59.8%) | 0.631 |
| Morphology* Pediculated Sessile Flat | 32 (19%) 126 (75%) 10 (6%) | 18 (15.9%) 90 (79.6%) 5 (4.5%) | 14 (25.5%) 36 (65.5%) 5 (9%) | 0.128 |
| Size** < 10 mm ≥ 10 mm | 220 (79.1%) 58 (20.9%) | 148 (78.7%) 40 (21.3%) | 72 (80%) 18 (20%) | 0.806 |
| Adenoma detection rate | 37.8% | 46.4% | 27.5% | < 0.001 |
Finally, we conducted three multivariable analyses. The first model included age, sex, smoking, MAFLD criteria, overweight, diabetes, hemoglobin, triglycerides, fasting glucose, glycosylated hemoglobin, and creatinine. As result, we observed that the presence of MAFLD was associated with a higher risk of having CRA [odds ratio (OR) = 2.50; 95%CI: 1.24-5.04; P = 0.011] [Table 4]. Serum creatinine was also statistically associated with CRA in Model 1. The second model excluding laboratory tests demonstrated that MAFLD criteria, age, and male gender were associated with detection of CRA [Table 4]. The final model only included the significant variables of Models 1 and 2 and showed that MAFLD criteria better predicts the presence of CRA (OR = 2.32; 95%CI: 1.68-3.19; P < 0.0001). The main variables of univariate and multivariable analysis are summarized in Table 4.
The multivariable analysis to assess the colorectal adenoma risk
| Variable | Univariate analysis | Multivariable analysis Model 1a | Multivariable analysis Model 2b | Multivariable analysis Model 3 | ||||||||
| OR | 95%CI | P-value | OR | 95%CI | P-value | OR | 95%CI | P-value | OR | 95%CI | P-value | |
| Age | 1.03 | 1.01-1.05 | < 0.0001 | 1.01 | 0.97-1.04 | 0.701 | 1.05 | 1.03-1.07 | < 0.001 | 1.03 | 1.01-1.05 | < 0.0001 |
| Male gender | 1.53 | 1.17-2.01 | 0.002 | 1.56 | 0.70-3.50 | 0.276 | 1.81 | 1.28-2.57 | 0.001 | 1.56 | 1.06-2.30 | 0.025 |
| Smoking | 1.45 | 1.06-1.98 | 0.022 | 1.07 | 0.55-2.11 | 0.905 | 1.40 | 0.96-2.05 | 0.084 | - | - | - |
| MAFLD criteria | 2.24 | 1.70-2.96 | < 0.0001 | 2.50 | 1.24-5.04 | 0.011 | 2.34 | 1.61-3.41 | < 0.0001 | 2.32 | 1.68-3.19 | < 0.0001 |
| Overweight | 2.30 | 1.48-3.58 | < 0.0001 | 1.06 | 0.40-2.84 | 0.905 | 1.53 | 0.92-2.53 | 0.102 | - | - | - |
| Diabetes | 1.89 | 1.22-2.93 | 0.004 | 1.64 | 0.67-4.03 | 0.282 | 1.28 | 0.74-2.21 | 0.375 | - | - | - |
| Ischemic stroke* | 4.39 | 1.16-16.66 | 0.018 | - | - | - | - | - | - | - | - | - |
| Creatinine (mg/dL) | 1.77 | 1.11-2.81 | 0.016 | 3.93 | 1.25-12.39 | 0.019 | - | - | - | 1.07 | 0.59-1.94 | 0.826 |
| Hemoglobin (g/dL) | 3.66 | 1.26-10.64 | 0.017 | 0.73 | 0.05-9.87 | 0.813 | - | - | - | - | - | - |
| Triglycerides (mg/dL) | 1.38 | 1.10-1.73 | 0.005 | 0.93 | 0.59-1.49 | 0.771 | - | - | - | - | - | - |
| Fasting blood glucose (mg/dL) | 5.79 | 2.89-11.61 | < 0.0001 | 2.66 | 0.47-14.94 | 0.266 | - | - | - | - | - | - |
| Glycosylated hemoglobin (%) | 1.42 | 1.06-1.89 | 0.018 | 0.95 | 0.55-1.63 | 0.841 | - | - | - | - | - | - |
| Total bilirubin (mg/dL) | 1.20 | 0.96-1.50 | 0.107 | - | - | - | - | - | - | - | - | - |
| γ-GT (U/L) | 1.16 | 0.99-1.37 | 0.070 | - | - | - | - | - | - | - | - | - |
| Hosmer-Lemeshow test P-value** | - | 0.745 | 0.182 | 0.548 | ||||||||
DISCUSSION
NAFLD and the recently proposed related entity MAFLD have been linked to an increased risk of CRA detection[32]. In the present study, we examined whether MAFLD is a risk factor for the detection of CRA in screening colonoscopies in a sample of Chilean Hispanic patients as no data exist on the association of fatty liver and CRA in Latin-American patients. We found that MAFLD was significantly associated with a higher risk of having CRA with an OR of 2.50. This finding was consistent in different models. Moreover, the ADR in patients with MAFLD (46.4%) was significantly higher than that observed in patients without MAFLD (27.5%).
The risk of CRA and CRC is influenced by both genetic and environmental factors. Genetic predisposition and familial syndromes increase the risk strikingly, but, in clinical practice, the majority of CRC correspond to sporadic rather than familial cases. Modifiable risk factors for CRC include smoking, overweight, a sedentary lifestyle, and an unhealthy low-fiber diet with high content of red and processed meat[33]. Obesity and overweight are also known risk factors for CRC[34-36]. Pathophysiological links between obesity and CRC are complex and may be related to the altered metabolic milieu commonly present in obese patients[37].
Our findings are in agreement with available data on the association between MAFLD and CRA. Prior evidence using the diagnosis of NAFLD suggests that the association is consistent[16,38-40]. However, most of the published studies include Asian patients and few studies have been carried out in the western population. Since the prevalence of NAFLD/MAFLD in Latin America is among the highest in the world[41], demonstrating its association with CRA is an important piece of evidence that can impact patient management. In our study, we did not find a significant association with an increased risk of advanced CRA according to the presence of MAFLD, which could be due to the low prevalence of these lesions in our study. Indeed, the incidence of CRC among individuals who undergo surveillance was lower than a prior Chilean study carried out during 2012-2015[42].
Although causality cannot be inferred from this study, the biological plausibility of the associations between MAFLD and CRA is generally accepted. Both conditions are related to unhealthy lifestyles including fructose-rich diets, processed meat consumption, sedentary habits, and the root cause of MAFLD, namely insulin resistance. Most of the proposed mechanisms that relate NAFLD and CRA, CRC, and other extrahepatic neoplasms suggest that the low-grade pro-inflammatory state generated by insulin resistance promotes neoplasia, but there are still a number of missing links[43]. Although insulin resistance was not associated with CRA in the present study, other conditions linked to insulin resistance, such as obesity, diabetes, and MAFLD, had a higher risk of CRA. This finding could be partially due to the progression from insulin resistance to diabetes or other conditions, with consequent cumulative damage. The potential dysregulation of bile acid metabolism has been suggested as one of the potential links based on data generated in mouse models[44-46], but more studies are needed.
The average age of patients included was 60 years or higher in the older population. This is attributable to the exclusive inclusion of patients who underwent screening colonoscopies. During the study period, the recommendations for surveillance of CRC in Chile were the onset of screening at 50 years[42]. Age is a key factor for the development of CRA as well as MAFLD, which could explain the high CRA rate and MAFLD prevalence identified in this study. On the other side, the most recent colorectal cancer screening guidelines recommend the onset of screening at 45 years[11]. From a public health perspective, the association between MAFLD and CRA could also modify the age of onset. Since other conditions (such as inflammatory bowel disease) have a high inflammation burden and long-term exposition[47], exposure over time could be necessary for patients with MAFLD to develop CRA and CRC. Future prospective studies are needed to elucidate this aspect and determine the best recommendations for surveillance.
The analysis of patients with colonoscopy performed only for screening purposes is one of the main strengths of the study. In addition, this is the first study on the Latin-American population that seeks to evaluate whether there is an association between colorectal adenomas and fatty liver disease associated with metabolic dysfunction. However, this study has some limitations. One of the most important ones is its retrospective nature, with the potential risk of lack of registry in some variables. Additionally, not all patients who underwent screening colonoscopy at these centers had abdominal imaging available, had different imaging methods, and the interval between both may also introduce risk of bias. In addition, withdrawal time was registered including the time of polypectomy, undoubtedly overestimating the relationship between withdrawal time and detection of CRA. Although a reverse association between MAFLD and CRA is plausible, it cannot be properly assessed in our study due to its nature. Even though this study demonstrated an association between MAFLD and the detection of CRA, it is unclear whether MAFLD could increase colorectal cancer risk.
In conclusion, the present study shows that Hispanic patients with MAFLD could be considered as a group with a high risk of presenting precursor lesions of colorectal cancer and that the ADR is significantly higher in this patient population. Thus, the presence of MAFLD should be taken into consideration when planning CRC screening strategies according to individual risk. We did not find statistically significant differences regarding size, number, morphology, location, or risk histology in adenomas of patients with MAFLD vs. patients without demonstrated hepatic steatosis.
DECLARATIONS
Authors’ contributionsContributed to the conception and design of the study, acquisition of data, and analysis and interpretation of data: Villalón A, Fuentes-López E, Villalón J, Villalón F, Yañez B, Díaz LA, Candia R, Arrese M
Contributed to drafting the article or revising it critically for important intellectual content: Villalón A, Ayares G, Díaz LA, Arrese M, Arab JP
All authors approved the final version to be submitted.
Availability of data and materialsNot applicable.
Financial support and sponsorshipThis work was partially funded by the Chilean government through the Fondo Nacional de Desarrollo
All authors declared that there are no conflicts of interest.
Ethical approval and consent to participateThis study was approved by the Institutional Review Board at the P. Univ. Catolica de Chile, Santiago, Chile (ID: 210309004). Individual informed consent waiver was granted by the local IRB.
Consent for publicationNot applicable.
Copyright© The Author(s) 2022.
Supplementary MaterialsREFERENCES
1. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2018;68:394-424.
2. Sierra MS, Forman D. Burden of colorectal cancer in Central and South America. Cancer Epidemiol 2016;44 Suppl 1:S74-81.
3. Ríos JA, Barake MF, Arce MJ, et al. [The present situation of colorectal cancer in Chile]. Rev Med Chil 2020;148:858-67.
4. Leslie A, Carey FA, Pratt NR, Steele RJ. The colorectal adenoma-carcinoma sequence. Br J Surg 2002;89:845-60.
5. Carballal S, Moreira L, Balaguer F. Serrated polyps and serrated polyposis syndrome. Cir Esp 2013;91:141-8.
6. Shussman N, Wexner SD. Colorectal polyps and polyposis syndromes. Gastroenterol Rep (Oxf) 2014;2:1-15.
7. Mangas-sanjuan C, Jover R, Cubiella J, et al. Endoscopic surveillance after colonic polyps and colorrectal cancer resection. 2018 update. Gastroenterol Hepatol (English Edition) 2019;42:188-201.
8. Dekker E, Tanis PJ, Vleugels JLA, Kasi PM, Wallace MB. Colorectal cancer. Lancet 2019;394:1467-80.
9. Nishihara R, Wu K, Lochhead P, et al. Long-term colorectal-cancer incidence and mortality after lower endoscopy. N Engl J Med 2013;369:1095-105.
10. Mandel JS, Church TR, Ederer F, Bond JH. Colorectal cancer mortality: effectiveness of biennial screening for fecal occult blood. J Natl Cancer Inst 1999;91:434-7.
11. Shaukat A, Kahi CJ, Burke CA, Rabeneck L, Sauer BG, Rex DK. ACG Clinical Guidelines: colorectal cancer screening 2021. Am J Gastroenterol 2021;116:458-79.
12. Rex DK, Schoenfeld PS, Cohen J, et al. Quality indicators for colonoscopy. Am J Gastroenterol 2015;110:72-90.
13. Younossi Z, Tacke F, Arrese M, et al. Global perspectives on nonalcoholic fatty liver disease and nonalcoholic steatohepatitis. Hepatology 2019;69:2672-82.
14. Kim GA, Lee HC, Choe J, et al. Association between non-alcoholic fatty liver disease and cancer incidence rate. J Hepatol 2017;S0168-8278(17)32294-8.
15. Chen W, Wang M, Jing X, et al. High risk of colorectal polyps in men with non-alcoholic fatty liver disease: a systematic review and meta-analysis. J Gastroenterol Hepatol 2020;35:2051-65.
16. Blackett JW, Verna EC, Lebwohl B. Increased prevalence of colorectal adenomas in patients with nonalcoholic fatty liver disease: a cross-sectional study. Dig Dis 2020;38:222-30.
17. Eslam M, Sanyal AJ, George J. International Consensus Panel. MAFLD: a consensus-driven proposed nomenclature for metabolic associated fatty liver disease. Gastroenterology 2020;158:1999-2014.e1.
18. Fouad Y, Waked I, Bollipo S, Gomaa A, Ajlouni Y, Attia D. What's in a name? Liver Int 2020;40:1254-61.
19. Dulai PS, Sandborn WJ, Gupta S. Colorectal cancer and dysplasia in inflammatory bowel disease: a review of disease epidemiology, pathophysiology, and management. Cancer Prev Res (Phila) 2016;9:887-94.
20. Lai EJ, Calderwood AH, Doros G, Fix OK, Jacobson BC. The Boston bowel preparation scale: a valid and reliable instrument for colonoscopy-oriented research. Gastrointest Endosc 2009;69:620-5.
21. Johnson CM, Wei C, Ensor JE, et al. Meta-analyses of colorectal cancer risk factors. Cancer Causes Control 2013;24:1207-22.
22. Dong Y, Liu Y, Shu Y, et al. Link between risk of colorectal cancer and serum vitamin E levels: a meta-analysis of case-control studies. Medicine (Baltimore) 2017;96:e7470.
23. Kobiela J, Dobrzycka M, Jędrusik P, et al. Metformin and colorectal cancer - a systematic review. Exp Clin Endocrinol Diabetes 2019;127:445-54.
24. Dobrzycka M, Spychalski P, Łachiński AJ, Kobiela P, Jędrusik P, Kobiela J. Statins and colorectal cancer - a systematic review. Exp Clin Endocrinol Diabetes 2020;128:255-62.
25. Guo CG, Ma W, Drew DA, et al. Aspirin use and risk of colorectal cancer among older adults. JAMA Oncol 2021;7:428-35.
26. Lee S, Kim BG, Kim JW, et al. Obstructive sleep apnea is associated with an increased risk of colorectal neoplasia. Gastrointest Endosc 2017;85:568-73.e1.
27. Niederseer D, Stadlmayr A, Huber-Schönauer U, et al. Cardiovascular risk and known coronary artery disease are associated with colorectal adenoma and advanced neoplasia. J Am Coll Cardiol 2017;69:2348-50.
28. Lasa J, Rausch A, Bracho LF, et al. Colorectal adenoma risk is increased among recently diagnosed adult celiac disease patients. Gastroenterol Res Pract 2018;2018:6150145.
29. Eslam M, Newsome PN, Sarin SK, et al. A new definition for metabolic dysfunction-associated fatty liver disease: an international expert consensus statement. J Hepatol 2020;73:202-9.
30. Hydes T, Brown E, Hamid A, Bateman AC, Cuthbertson DJ. Current and emerging biomarkers and imaging modalities for nonalcoholic fatty liver disease: clinical and research applications. Clin Ther 2021;43:1505-22.
31. Hidalgo B, Goodman M. Multivariate or multivariable regression? Am J Public Health 2013;103:39-40.
32. Seo JY, Bae JH, Kwak MS, et al. The risk of colorectal adenoma in nonalcoholic or metabolic-associated fatty liver disease. Biomedicines 2021;9:1401.
33. Thune I, Allen K, Thompson RL, Wiseman MJ, Mitrou PN, McGinley-Gieser D. Abstract P3-10-06: what is the latest evidence on diet, nutrition, physical activity and cancer - key findings from the WCRF/AICR continuous update project. Cancer Res 2018:78.
34. Chen X, Liang H, Song Q, Xu X, Cao D. Insulin promotes progression of colon cancer by upregulation of ACAT1. Lipids Health Dis 2018;17:122.
35. Aslan A, Erdem H, Celik MA, Sahin A, Cankaya S. Investigation of insulin-like growth factor-1 (IGF-1), P53, and Wilms' tumor 1 (WT1) expression levels in the colon polyp subtypes in colon cancer. Med Sci Monit 2019;25:5510-7.
37. Mili N, Paschou SA, Goulis DG, Dimopoulos MA, Lambrinoudaki I, Psaltopoulou T. Obesity, metabolic syndrome, and cancer: pathophysiological and therapeutic associations. Endocrine 2021;74:478-97.
38. Hwang ST, Cho YK, Park JH, et al. Relationship of non-alcoholic fatty liver disease to colorectal adenomatous polyps. J Gastroenterol Hepatol 2010;25:562-7.
39. Chen QF, Zhou XD, Sun YJ, et al. Sex-influenced association of non-alcoholic fatty liver disease with colorectal adenomatous and hyperplastic polyps. World J Gastroenterol 2017;23:5206-15.
40. Chen J, Bian D, Zang S, et al. The association between nonalcoholic fatty liver disease and risk of colorectal adenoma and cancer incident and recurrence: a meta-analysis of observational studies. Expert Rev Gastroenterol Hepatol 2019;13:385-95.
41. Araújo AR, Rosso N, Bedogni G, Tiribelli C, Bellentani S. Global epidemiology of non-alcoholic fatty liver disease/non-alcoholic steatohepatitis: what we need in the future. Liver Int 2018;38 Suppl 1:47-51.
42. López-Kostner F, Zárate AJ, Ponce A, et al. [Results of a multicentric colorectal cancer screening program in Chile]. Rev Med Chil 2018;146:685-92.
43. Chakraborty D, Wang J. Nonalcoholic fatty liver disease and colorectal cancer: correlation and missing links. Life Sci 2020;262:118507.
44. Gadaleta RM, Garcia-Irigoyen O, Moschetta A. Bile acids and colon cancer: is FXR the solution of the conundrum? Mol Aspects Med 2017;56:66-74.
45. Degirolamo C, Modica S, Palasciano G, Moschetta A. Bile acids and colon cancer: solving the puzzle with nuclear receptors. Trends Mol Med 2011;17:564-72.
46. Arab JP, Karpen SJ, Dawson PA, Arrese M, Trauner M. Bile acids and nonalcoholic fatty liver disease: molecular insights and therapeutic perspectives. Hepatology 2017;65:350-62.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Villalón A, Díaz LA, Fuentes-López E, Villalón J, Villalón F, Ayares G, Yañez B, Candia R, Arab JP, Arrese M. Colorectal adenomas and MAFLD: a cross-sectional study in a Hispanic screening cohort. Metab Target Organ Damage 2022;2:3. http://dx.doi.org/10.20517/mtod.2021.17
AMA Style
Villalón A, Díaz LA, Fuentes-López E, Villalón J, Villalón F, Ayares G, Yañez B, Candia R, Arab JP, Arrese M. Colorectal adenomas and MAFLD: a cross-sectional study in a Hispanic screening cohort. Metabolism and Target Organ Damage. 2022; 2(1): 3. http://dx.doi.org/10.20517/mtod.2021.17
Chicago/Turabian Style
Villalón, Alejandro, Luis Antonio Díaz, Eduardo Fuentes-López, Javier Villalón, Fernando Villalón, Gustavo Ayares, Bárbara Yañez, Roberto Candia, Juan Pablo Arab, Marco Arrese. 2022. "Colorectal adenomas and MAFLD: a cross-sectional study in a Hispanic screening cohort" Metabolism and Target Organ Damage. 2, no.1: 3. http://dx.doi.org/10.20517/mtod.2021.17
ACS Style
Villalón, A.; Díaz LA.; Fuentes-López E.; Villalón J.; Villalón F.; Ayares G.; Yañez B.; Candia R.; Arab JP.; Arrese M. Colorectal adenomas and MAFLD: a cross-sectional study in a Hispanic screening cohort. Metab Target Organ Damage. 2022, 2, 3. http://dx.doi.org/10.20517/mtod.2021.17
About This Article
Copyright
Data & Comments
Data
 Cite This Article 22 clicks
Cite This Article 22 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.